Changing Behavior Can Be Challenging

Changing Behavior Can Be Challenging


As clinicians, we do our best to provide quality patient care. We study in school to pass boards and then continue to read journals, participate in continuing education, and some even conduct research. All this is to practice evidence-based medicine. However, there are a number of tasks clinicians perform that could be done better. By better, I don’t mean doing a task better. I mean using data and technology to BE better. Yet, changing behavior is a challenge. This blog will focus on three ways we should consider changing behavior to be better: range of motion, manual muscle testing, and joint assessment. I understand there are some really fabulous clinicians out there with exceptional skills. You may be one of them. But, we are all human and we have limitations on what we can see with the naked eyes and feel with our hands.
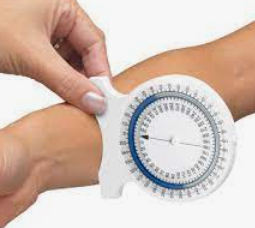
 Range of Motion (ROM) – goniometers are the standard tool for the assessment of ROM. They have progressed to include “bubbles” to level the device with the fixed segment. They are now available in electronic versions as well as in mobile apps. Studies have supported these devices to provide accurate data. Research has demonstrated digital inclinometers are a more accurate method of assessment (6° minimum significant difference) of knee range of motion than long arm goniometers (minimum significant different of 10°). Of the technique of the user can also be problematic. But even more of a problem is when people try to “eye-ball” ROM. This is not objective data.
Range of Motion (ROM) – goniometers are the standard tool for the assessment of ROM. They have progressed to include “bubbles” to level the device with the fixed segment. They are now available in electronic versions as well as in mobile apps. Studies have supported these devices to provide accurate data. Research has demonstrated digital inclinometers are a more accurate method of assessment (6° minimum significant difference) of knee range of motion than long arm goniometers (minimum significant different of 10°). Of the technique of the user can also be problematic. But even more of a problem is when people try to “eye-ball” ROM. This is not objective data.
Manual Muscle Test (MMT) – likewise, MMT with our hands has been shown in several studies to have limitations. The first is the ability to place a value on the force a person is able to resist. Even with the (+) and (-) descriptors, the scale of 0 to 5 only makes sense of values up to 3+ (some resistance against gravity). Once a person is able to complete the ROM against gravity, the assessment becomes subjective. How much resistance is a 4 versus a 4+? Muscle testing grades of 4(-), 4, 4(+), and 5 are highly variable. Numbers displayed on a dynamometer are much more discerning when it comes to assessing both current status and progress. Being able to calculate a percentage of strength deficits and improvements in strength gains allow for the documentation of objective data. These are both examples demonstrating how technology can provide precise measurements for better patient care.
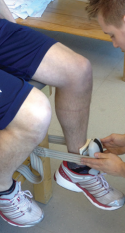 Furthermore, studies have shown the ability to apply force is limited by the strength of the clinician. If the clinician’s upper body strength is not able to “break” the knee extension force of a client, how can strength be adequately assessed? Thus, hand-held dynamometer (HHD) are essential. This is the only way to obtain objective data. One still needs to appreciate that the objective data can be limited to the strength of the clinician. This is where some creativity needs to come into play. The use of straps to enable maximal resistance can be very valuable. Justification of the need for ongoing treatment and the ability to compare side-to-side strength can only be done with objective data.
Furthermore, studies have shown the ability to apply force is limited by the strength of the clinician. If the clinician’s upper body strength is not able to “break” the knee extension force of a client, how can strength be adequately assessed? Thus, hand-held dynamometer (HHD) are essential. This is the only way to obtain objective data. One still needs to appreciate that the objective data can be limited to the strength of the clinician. This is where some creativity needs to come into play. The use of straps to enable maximal resistance can be very valuable. Justification of the need for ongoing treatment and the ability to compare side-to-side strength can only be done with objective data.
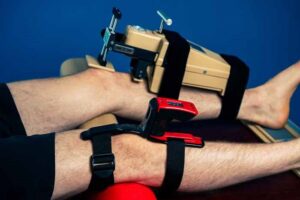 Joint Assessment – with only one exception, joint assessment has always been done with our hands. We wiggle a joint and say “that feels loose.” The invention of the KT1000 in the 1980’s allows us to objectify knee cruciate ligament laxity for the first time. Yes, there were “issues.” The handle pulled the device away for the tibia when performing the anterior translation and the measure represented a larger magnitude of displacement than was actually occurring. However, when compared to the uninvolved knee, the “error” was washed out. The KT1000 has not been available since 2012 but was replaced by the Mobil-Aider Arthrometer in 2021. It is able to assess the ACL, as well as shoulders, elbows, wrists, and ankles. Now clinicians have a tool to assess joint laxity and quantify joint mobilization techniques. Yes, we have done all of these things with our hands for decades but can you really feel a 1-2 mm difference in linear translation with your hands? What about serial measurements? Wouldn’t it be helpful to be able to quantify improvements in arthrokinematics motion with an arthrometer just like we quantify osteokinematic motion with a goniometer?
Joint Assessment – with only one exception, joint assessment has always been done with our hands. We wiggle a joint and say “that feels loose.” The invention of the KT1000 in the 1980’s allows us to objectify knee cruciate ligament laxity for the first time. Yes, there were “issues.” The handle pulled the device away for the tibia when performing the anterior translation and the measure represented a larger magnitude of displacement than was actually occurring. However, when compared to the uninvolved knee, the “error” was washed out. The KT1000 has not been available since 2012 but was replaced by the Mobil-Aider Arthrometer in 2021. It is able to assess the ACL, as well as shoulders, elbows, wrists, and ankles. Now clinicians have a tool to assess joint laxity and quantify joint mobilization techniques. Yes, we have done all of these things with our hands for decades but can you really feel a 1-2 mm difference in linear translation with your hands? What about serial measurements? Wouldn’t it be helpful to be able to quantify improvements in arthrokinematics motion with an arthrometer just like we quantify osteokinematic motion with a goniometer?
The desire to contribute to the enhancement of objectivity in orthopedics has led me along a fascinating (and somewhat tumultuous) journey to develop the Mobil-Aider arthrometer. Through years of teaching orthopedic manual skills and clinical practice, I struggled with the fact that there was no device to quantify joint mobility. Studies have reported fair to good intra-rater reliability but poor inter-rater reliability. Thus, each person may be consistent but between people, there is great variability. Replicating techniques become a significant problem when trying to assess the effectiveness of manual therapy interventions. If you take a CPR course, you do manual compressions until you hear a “click.” That auditory feedback lets you know you are pushing to sufficient depth. If you don’t hear a “click,” you know to push harder. Immediate auditory or visual feedback is very important in skill acquisition.4 So why can’t we quantify joint mobility?
My experience in the academic lab included instructing students in manual techniques. I demonstrated the task. They mimic what I did while I provided feedback.
Problem 1: I had no way of knowing the feel of their grip or the magnitude of the translation if they were not do the technique on me.
Problem 2: I had no way of knowing what they were feeling and they struggled to explain it.
Imagine a student (or novice clinician) doing an inferior glide of the shoulder. I would ask, “Do you feel the capsular endfeel?” “Do you feel how the inferior glide comes to a soft stop but as you maintain consistent pressure, the glide creeps a little more?” Of course, if you have felt this before, you understand the description and how to perform the task. However, if you have not, it can be challenging to appreciate the “feel.” If the student had a device interfaced between their hands and the patient (or lab partner) and if one were able to say, “when you get to 5 mm of translation, do you feel how you begin to encounter some resistance to the inferior glide?” The student would then be instructed to maintain the pressure and watch the numbers on the arthrometer increase by 0.5 to 1 mm as the “creep” of the capsular endfeel occurs. With the “coaching” and the visual feedback, the mastery of the psychomotor task is enhanced. Equally as important, the student would now have a way to continue to practice correctly when the faculty member is not present. This was the driving force for the development of the Mobil-Aider arthrometer.
Through the development process (funded by the National Science Foundation), I learned about customer acquisition and the value of listening to the pain points of the consumer. This is where the scope of the Mobil-Aider expanded into ligamentous stability testing. There have now been over a dozen studies published on validity/reliability and clinical application. I would like to highlight two studies that are important in appreciating the value of technology and obtaining objective data.
One study was “Use of a New Arthrometer to Assess Knee Pathology.” The Lachman test was used with the Mobil-Aider to examine ACL laxity. The mean difference between the involved and uninvolved knees were -0.18, 2.05, and 3.38 mm for intact, partial tear, and complete tear as identified on MRI, respectively. Thus, the Mobil-Aider allowed the user to distinguish millimeters of differences between extremities. This is valuable information. Many of you may remember the KT1000 device. It was a large apparatus (fit in a roller bag type case) that could only be used on the knee. It also had several problems. There was a hard plastic piece that had to be pressed down onto the patella for stabilization and the handle used for the tibial translation pulled the device away for the tibia (introducing measurement error). The Mobil-Aider design addressed these points and is valid within 5% of measurement.
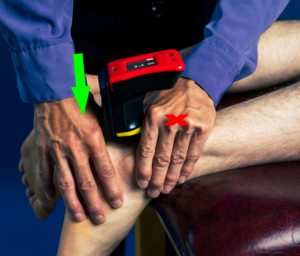 Likewise, a study entitled “Assessing Lateral Ankle Sprains with a New Arthrometer” identified significant differences between the control and grade I and grade II ankle sprain groups. There was ± 0.31 mm difference in anterior translation (anterior drawer) between healthy ankles. Whereas there was 1.11 mm and 2.16 mm difference between ankles in grade I and grade II sprains, respectively. This is consistent with stress radiographs. Despite the manual anterior drawer test being convenient, the subjectivity makes it unreliable. A difference of a bit over 1 millimeter could impact the clinical decision to treat with an aircast versus a boot. By comparing the data of the injured to uninjured extremity, we mitigate the variability of what is “normal.”
Likewise, a study entitled “Assessing Lateral Ankle Sprains with a New Arthrometer” identified significant differences between the control and grade I and grade II ankle sprain groups. There was ± 0.31 mm difference in anterior translation (anterior drawer) between healthy ankles. Whereas there was 1.11 mm and 2.16 mm difference between ankles in grade I and grade II sprains, respectively. This is consistent with stress radiographs. Despite the manual anterior drawer test being convenient, the subjectivity makes it unreliable. A difference of a bit over 1 millimeter could impact the clinical decision to treat with an aircast versus a boot. By comparing the data of the injured to uninjured extremity, we mitigate the variability of what is “normal.”
Both of these studies are just the beginning of the potential to populate the literature with objective data about joint mobility/laxity. The use of the Mobil-Aider arthrometer is the future of evidence-based orthopedics.
Summary
We have to do better! We will struggle to progress our patients AND the profession if we keep doing what we always do. Data provides information upon which we make decisions. Data tells us when a patient is progressing or regressing. Data can provide normative standards to which a patient’s status can be compared. Challenge yourself to be better!
For more information about evidence-based orthopedic clinical tests or manual techniques please subscribe to iOrtho+ PREMIUM app at: https://iortho.xyz/
If you would like to learn more about the Mobil–Aider orthopedic measurement device to quantify joint mobility, please visit: https://mobil-aider.com/
- Hancock GE, Hepworth T, Wembridge K. Accuracy and reliability of knee goniometer methods. BMC Musculoskeletal Disorders. 2013;14(17)
- Cadogan A, Laslett M, Hing W, McNair P, Williams M. Reliability of a new hand-held dynamometer in measuring shoulder range of motion and strength. Manual Therapy. 2011; 16(1):97–101.
- Romero-Franco N, Fernandez-Dominguez JC, Montano-Munuera JA, Romero-Franco J, Jimenez-Reyes P. Validity and reliability of a low-cost dynamometer to assess maximal isometric strength of upper limb. Journal of Sports Science. 2019;37(15):1787–1793.
- Wulf G, Shea C, Lewthwaite R. Motor skills learning and performance: A review of influential factors. Medical Education. 2010;44(1):75-84.
- Hammoud S, Palombaro K, Gulick DT. Use of a New Arthrometer to Assess Knee Pathology. Global Journal of Orthopedic Research. January 2022
- Taweel NR, Gulick DT, Palombaro KM. Assessing Lateral Ankle Sprains with a New Arthrometer. March 2022, publication pending
