Sharing a Clinical Problem-Solving Scenario



Sharing a Clinical Problem-Solving Scenario
 Many times I find myself in situations where I wish I could record an athlete/client interaction because of the opportunity for it to be a teachable moment. Students and novice practitioners could benefit from seeing the clinical problem-solving process. Although I did not record it, I thought I would share the scenario via a BLOG.
Many times I find myself in situations where I wish I could record an athlete/client interaction because of the opportunity for it to be a teachable moment. Students and novice practitioners could benefit from seeing the clinical problem-solving process. Although I did not record it, I thought I would share the scenario via a BLOG.
***Two points of interest: 1) there is no personal information disclosed to violate confidentiality and 2) this was a field evaluation not a clinical one.
History:
Client: 12-year-old female field hockey player. Reports several months of knee “popping.” She indicates there was no trauma and it occurs bilaterally. She stated she never had a lower extremity injury.
Visual Inspection:
Clinician: Pre-pubescent child who is thin with no edema, no ecchymosis, no scars or rashes. Mild genu valgus in standing.
Interview:
Clinician: Can you tell me if you have had any other medical issues (illnesses)? Do you take any medication(s)?
Client: No medical issues, no medication
Clinician: Have you ever injured your legs before?
Client: No
Clinician: Have you seen any medical providers about this problem?
Client: Yes, I went to “urgent care.” They recommended I get an x-ray but my mom has not set that up yet.
Physical Observation:
Clinician: Can you bend and straighten your knee as far as possible for me please?
Client: (In sitting) She flexes and extends through full range of motion but a visual “shift” was noted.
Clinician: Did that hurt?
Client: No
Clinician: Can you go through that same knee motion in standing, i.e. a squat?
Client: (In self-selected foot position, narrow base of support that was less than shoulder width) Athlete performed the squat and completed the full squat with butt to the floor (NKA ass to grass but this a child and I thought that was tacky). A “pop” was experienced with the squat motion.
Clinician: Noted the knees went into dynamic valgus bilaterally. Did that hurt?
Client: No
Clinician: Can you do that squat again with your feet further apart and your toes turned outward?
Client: (Squat motion was repeated) No popping occurred and full range of motion was achieved.
Physical Examination:
Clinician: Performed bilaterally…
Range of motion: Hips, knees, and ankles are all within normal limits
Strength:
-
-
- Hips = weak abductors and external rotators; flexion and extension appeared age and body-type (ectomorph) appropriate
- Knees = within normal limited, no extensor lag on straight leg raise
- Ankle = within normal limited
-
Clinical tests:
-
-
- Valgus stress = (+)
- Varus stress = (-)
- Lachman test = (-)
- Patella mobility = (-) for pain reproduction with translation in all directions
- Thesally test = (-)
-
Palpation: 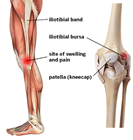
- Knee joint line tenderness = (-)
- Patella = (-) at rest and with knee flexion/extension
- Patella and quadriceps tendon = (-) at rest and with knee flexion/extension
- Tibial plateau = (-)
- Medial and lateral collateral ligaments = (-)
- Gerdy’s tubercle & slightly proximal = (-) at rest but (+) for snapping with non-weightbearing & weight-bearing knee flexion/extension
Assessment: Based on the history (lack of trauma, no medical issues), the visual inspection (no major alignment issues), the interview about the client’s sense of “popping” in the knee, and the physical examination with a palpable “snapping” sensation on the lateral aspect of the knee with flexion/extension at about the 30 degree position that could be mitigated with a change in hip position (abduction & ER) as well as weak hip muscular, a diagnosis iliotibial band (ITB) syndrome is reasonable.
Additional testing:
- Clinical tests to assess ITB tightness could include the Ober test. However, Willett et al (2016) refutes the hypothesis that ITB plays a role in limiting hip adduction during the Ober test. Their results suggest the Ober test assesses tightness of structures proximal to the hip joint, such as the gluteus medius and minimus muscles and the hip joint capsule, rather than the ITB. Statistical data for the Ober Test are as follows: Sensitivity = 89%, Specificity = 92%, Reliability (ICC) = 0.92
- Imaging such as T2 MRI could reveal thickening of the distal ITB thickening.
- Likewise, ultrasound can also be used to demonstrate ITB thickening
For more cutting-edge orthopedic information on iOrtho+ PREMIUM Mobile App, please visit https://iortho.xyz/
If you would like to learn more about the Mobil–Aider Orthopedic Arthrometer to quantify joint mobility, please visit: https://mobil-aider.com/
References:
- Cibere J, Thorne A, Bellamy N, et al. Reliability of the hip examination in osteoarthritis: effect of standardization. Arthritis Rheumatology. 2008;59:373-381
- Gajdosik R, Sandler MM, Marr HL. Influence of knee positions & gender on the Ober test for length of the iliotibial band. Clinical Biomechanics. 2003;18:77-79
- Gulick DT. iOrtho+ Mobile App. DTG Enterprises LLC. 2020
- Gulick, DT. OrthoNotes, 4th FA Davis Publishing, Philadelphia. 2018
- Melchione W, Sullivan S. Reliability of measurements obtained by use of an instrument designed to measure iliotibial band length indirectly. Journal Orthopedic & Sports Physical Therapy. 1993;18:511-515
- Ober FB: The role of the iliotibial and fascia lata as a factor in the causation of low-back disabilities and sciatica, Journal Bone Joint Surgery 1936;18:105-110
- Piva SR, Fitzgerald K, Irrgang JJ, et al. Reliability of measures of impairments associated with patellofemoral pain syndrome. BMC Musculoskeletal Disorders. 2006;7:33
- Reese N, Bandy W. Use of an inclinometer to measure flexibility of the iliotibial band using the Ober test & Modified Ober test. Journal Orthopedic & Sports Physical Therapy. 2003;33:326-330
- Willett GM, Keim SA, Shostrom VK, Lomneth CS. An Anatomic Investigation of the Ober Test. American Journal of Sports Medicine. 2016;44(3):696-701
