The “Other” Cruciate Ligament, AKA PCL
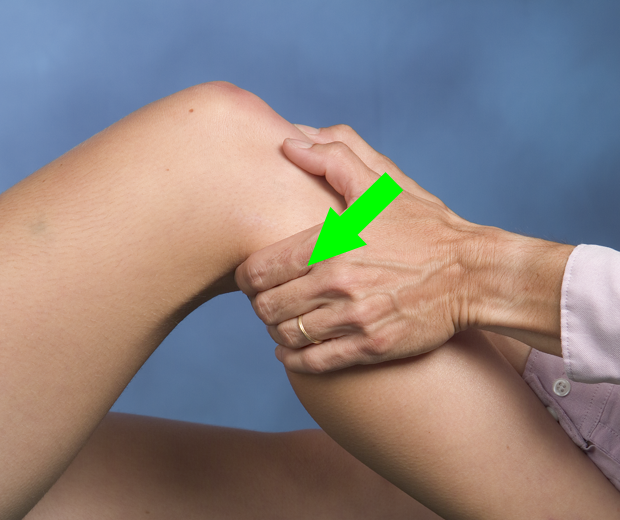


The “Other” Cruciate Ligament, AKA the Posterior Cruciate Ligament (PCL)
When someone says they injured their cruciate ligament, the first thought is the anterior cruciate. Of course it is the most common cruciate to injure, but what about the “other” cruciate ligament: the posterior cruciate? The posterior cruciate (PCL) is composed of two bands that blend together. It attaches to the posterior intercondylar area and passes anterosuperiorly to insert into the lateral surface of the medial femoral condyle. The PCL is responsible for posterior translation of the tibia on the femur in open kinetic chain and anterior translation of the femur on the tibia in closed kinetic chain.
The PCL is about the thickness of your pinky finger. Injury of the PCL typically requires a powerful force. Injury may occur via:
- Direct blow to the anterior knee (tibial tuberosity) in flexion, i.e. dashboard of a car, fall on a flexed knee
- Hyperextension of the knee
- Misstep, i.e. miscalculation when stepping down off a curb or on/off a moving object like a boat
Although PCL tears tend to be partial with the potential to heal on their own, the symptoms may include:
- Rapid swelling (because of the vascularization of the ligament)
- Knee stiffness
- Antalgic gait
- Feeling of instability or “giving way”
- Difficulty kneeling
There are three tests used to assess the PCL:
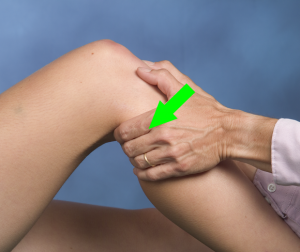 The posterior drawer test is simply the opposite of the anterior drawer used for the anterior cruciate ligament (ACL). The patient lies supine with the knee flexed to 80-90°. The clinician wraps his/her hands around the proximal knee with the thumbs palpating the joint line and the fingers palpating the hamstring tendons to confirm they are relaxed. A posterior force is applied to the anterior tibia. Excessive posterior excursion, when compared to the contralateral limb, is a positive test. As a clinician it may be challenging to assess millimeters of difference in the magnitude of posterior translation between the knees but a soft or empty endfeel may also be present.
The posterior drawer test is simply the opposite of the anterior drawer used for the anterior cruciate ligament (ACL). The patient lies supine with the knee flexed to 80-90°. The clinician wraps his/her hands around the proximal knee with the thumbs palpating the joint line and the fingers palpating the hamstring tendons to confirm they are relaxed. A posterior force is applied to the anterior tibia. Excessive posterior excursion, when compared to the contralateral limb, is a positive test. As a clinician it may be challenging to assess millimeters of difference in the magnitude of posterior translation between the knees but a soft or empty endfeel may also be present.
The test is easy to perform and the statistics are strong:
- Sensitivity = 22-100%
- Specificity = 99-100%
- (+) LR = 90
- (-) LR = 0.10
- Reliability (Kappa) = 0.82
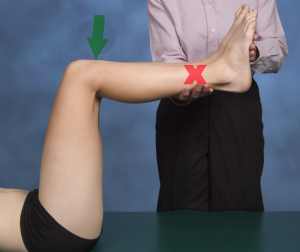 When performed in combination with the sag test, the sensitivity is 90% and the specificity is 99%. The sag test is performed in supine with both the hips and knees flexed to 90°. With the lower extremities supported distally, the level of the tibial tuberosity is compared. When the PCL is torn, the ipsilateral tibial tuberosity will be lower (sag back) than the contralateral side.
When performed in combination with the sag test, the sensitivity is 90% and the specificity is 99%. The sag test is performed in supine with both the hips and knees flexed to 90°. With the lower extremities supported distally, the level of the tibial tuberosity is compared. When the PCL is torn, the ipsilateral tibial tuberosity will be lower (sag back) than the contralateral side.
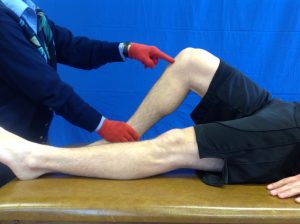 The third test is the active PCL drawer test. This test is performed in 45° of hip flexion and 90° of knee flexion. The distal tibia is stabilized while the patient is asked to contract the quadriceps muscle. A positive test is more anterior translation of the tibia on the ipsilateral side than the contralateral side. This occurs because the “drop back” position of the tibia when the PCL is injured. Although sensitivity is 54-98% and specificity is 97-100%, the clinician should be aware that the anterior translation with a quadriceps contraction could also be the result of an ACL tear. So a positive active PCL drawer should be confirmed with another positive PCL test. Endfeel may also provide valuable information. In other words:
The third test is the active PCL drawer test. This test is performed in 45° of hip flexion and 90° of knee flexion. The distal tibia is stabilized while the patient is asked to contract the quadriceps muscle. A positive test is more anterior translation of the tibia on the ipsilateral side than the contralateral side. This occurs because the “drop back” position of the tibia when the PCL is injured. Although sensitivity is 54-98% and specificity is 97-100%, the clinician should be aware that the anterior translation with a quadriceps contraction could also be the result of an ACL tear. So a positive active PCL drawer should be confirmed with another positive PCL test. Endfeel may also provide valuable information. In other words:
- excessive anterior excursion with a firm endfeel indicates the ACL is intact but the PCL may be injured
- excessive anterior excursion with a soft or empty endfeel may indicate an ACL injury
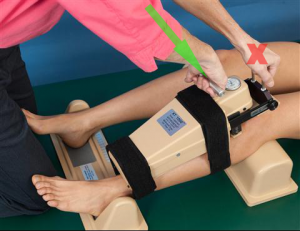 Another method used to assess the PCL is with an arthrometer. The KT1000 and KT2000 are no longer on the market but many are still in use. In supine, the patient is positioned with the knee between 20-35° of flexion and feet in the spacer device. A thigh strap is secured to control hip ER. The arthrometer is strapped onto the patient’s tibia with the axis aligned with the knee joint line. The dial is set to zero and the clinician pushes on the handle to apply a posterior translation of the tibia on the femur. Audible beeps correspond to the amount of force applied. Although a soft endfeel is indicative of a PCL injury, the ability to quantify the tibial displacement may be important. The KT1000/2000 manufacturer suggested a posterior translation 2 mm greater than the uninvolved knee or 10 mm of total posterior translation suggests a torn PCL. Literature on the KT1000/2000 has been variable. Some suggest a high false positive rate (some as high as 28%).
Another method used to assess the PCL is with an arthrometer. The KT1000 and KT2000 are no longer on the market but many are still in use. In supine, the patient is positioned with the knee between 20-35° of flexion and feet in the spacer device. A thigh strap is secured to control hip ER. The arthrometer is strapped onto the patient’s tibia with the axis aligned with the knee joint line. The dial is set to zero and the clinician pushes on the handle to apply a posterior translation of the tibia on the femur. Audible beeps correspond to the amount of force applied. Although a soft endfeel is indicative of a PCL injury, the ability to quantify the tibial displacement may be important. The KT1000/2000 manufacturer suggested a posterior translation 2 mm greater than the uninvolved knee or 10 mm of total posterior translation suggests a torn PCL. Literature on the KT1000/2000 has been variable. Some suggest a high false positive rate (some as high as 28%).
- Sensitivity = 65% at 89N of force and 73% at 134N of force
- 92% at maximal manual force
- Correlation to Radiographs = 0.67
In summary, there are three clinical tests with responsibly strong statistical values to support their use. As always, the clinician should look for multiple positive tests for a given structure to corroborate damage to a given tissue. Based on the mechanism of injury, one should also rule out associated tissues that could be involved.
For more cutting edge orthopedic information subscribe to iOrtho+ Premium Mobile App, at https://iortho.xyz The annual subscription rate is only $1.99 per month or $9.99 per year
- Arneja A, Leith J. Review article: Validity of the KT-1000 knee ligament arthrometer. Journal of Orthopaedic Surgery. 2009;17(1):77-79
- Baker CL, Norwood LA, Hughston JC. Acute combined posterior cruciate & posterolateral instability of the knee. American Journal of Sports Medicine. 1984;12(3):204-208
- Boyer P, Dijan P, Christel P, Paoletti X, Degeorges R. Reliability of the KT-1000 arthrometer (Medmetric) for measuring anterior knee laxity: comparison with Telos in 147 knees. Revue de chirurgie orthopédique et réparatrice de l’appareil moteur 2004;90(8):757-764
- Cibere J, Bellamy N, Thorne A, Esdaile JM, McGorm KJ, Chalmers A, et al. Reliability of the knee examination in osteoarthritis: effect of standardization. Arthritis Rheumatism. 2004;50:458-468
- Daniel DM, Stone ML, Barnett P et al: Use of the quadriceps active test to diagnose posterior cruciate ligament disruption and measure posterior laxity of the knee, J Bone Joint Surg Am. 1988; 70:386-391
- De Lee JC: Ligamentous injury of the knee. In Stanitski CL, DeLee JC, Drez D, editors: Pediatric and adolescent sports medicine, Philadelphia, 1994, WB Saunders.
- Ferrari DA, Ferrari JD, Coumas J: Posterolateral instability of the knee, Journal Bone Joint Surgery America 1994;76:187-192
- Fowler PJ, Messieh SS. Isolated posterior cruciate ligament injuries in athletes. American Journal Sports Medicine. 1987;15:553-557
- Gulick, DT. OrthoNotes, 4th FA Davis Publishing, Philadelphia 2018
- Gulick DT. iOrtho+ Mobile App. DTG Enterprises LLC 2020
- Loos WC, Fox JM, Blazina ME, Del Pizzo W, Friedman MJ. Acute posterior cruciate ligament injuries. American Journal of Sports Medicine. 1981;8(2):86-92
- Malanga GA, Andrus S, Nadler SF, McLean J. Physical examination of the knee: A review of the original test description & scientific validity of common orthopedic tests. Archives Physical Medicine Rehabilitation. 2003;84:592-603
- Muller W: The knee: form, function and ligament reconstruction, New York, 1983, Springer-Verlag.
- Rubinstein RA, Shelbourne KD, McCarroll JR, van Meter CD, Rettig AC. The accuracy of the clinical examination in the setting of posterior cruciate ligament injuries. American Journal of Sports Medicine. 1994;22:550-557
- Shelbourne KD, Benedict F, McCarroll JR et al: Dynamic posterior shift test: an adjuvant in evaluation of posterior tibial subluxation, American Journal Sports Medicine. 1989;17:275-277
- Shino K, Horibe S, Ono K: The voluntary evoked posterolateral drawer sign in the knee with posterolateral instability, Clinical Orthopedics 1987;215:179-186
- Staubi H-U, Jakob RP. Posterior instability of the knee near extension. Journal of Bone & Joint Surgery. 1990;72-B:225-230
- Veltri DM, Warren RF: Isolated and combined posterior cruciate ligament injuries, J Am Acad Orthop Surg. 1993; 1:67-75
